Why We Aren’t Using UV to Disinfect Everything—Yet
Negative perception and costs pose obstacles to a promising technology
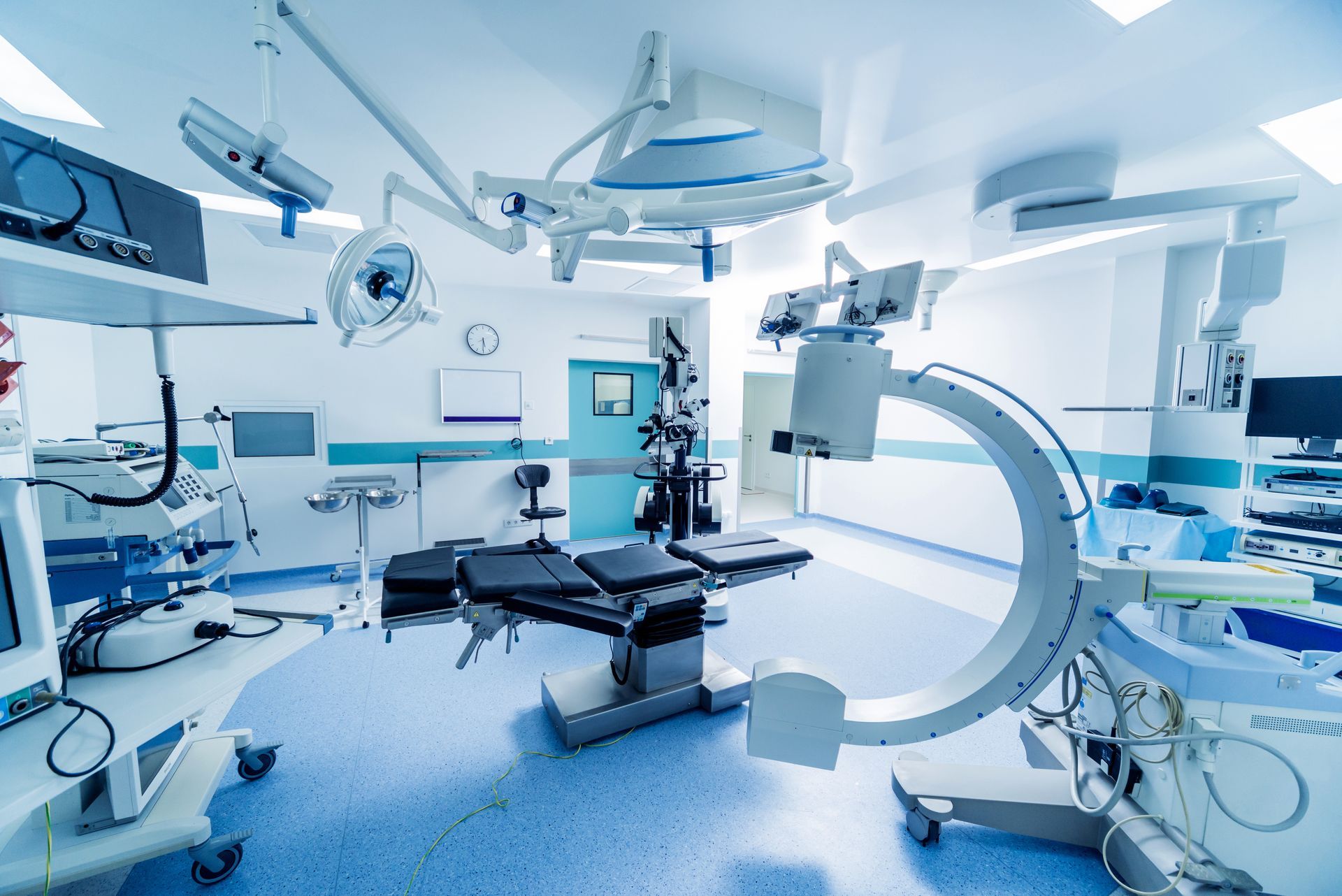
As the coronavirus pandemic continues, a technology that has existed for over 100 years is getting renewed attention as a promising disinfection tool. Ultraviolet germicidal radiation, which uses short-wavelength UV rays to kill bacteria and viruses, is already used to disinfect the air, water, and surfaces in limited settings. In May, a report by the Illuminating Engineering Society, an authority on lighting technology, showed that UV-C germicidal radiation can play a key role in inactivating the SARS-CoV-2 virus, which causes Covid-19. Now some companies whose products use this technology are seeing heightened interest.
“The manufacturers can’t keep up with the demand right now,” says Edward A. Nardell, a professor of medicine at Harvard Medical School. “You’re going to see UV widely used as we continue with this pandemic and have no treatment.” This technology has previously been used in health care settings and is a standard method of potable water treatment, but it hasn’t been widely embraced because of negative public perception and concerns about costs.
The technology’s roots date to 1877 when scientists observed that sunlight could prevent the growth of bacteria inside a test tube. Shortwave UV rays kill or inactivate microbes by damaging their DNA, rendering them incapable of replicating. The discovery helped to stop the spread of measles in schools in the ’40s and the transmission of tuberculosis, says Nardell, but the demand dissipated as vaccines for these diseases were developed.
Germicidal UV is now sometimes perceived negatively, he says, because people confuse it with the UV-A and UV-B rays that cause sun-related damage. Germicidal UV technology uses a shorter wavelength of radiation, called UV-C, which is also generated by the sun but gets absorbed in the atmosphere, so it doesn’t pose as much of a risk to people outdoors. But even though UV-C rays are far less dangerous than UV-A and UV-B, overexposure to it indoors is still risky, and it’s still not safe for humans to be present when UV-C technology is being used, says Peter Setlow, a professor of molecular biology and biophysics at UConn Health. The technology’s reputation recently suffered a further setback when President Trump suggested in a press briefing in April that shining heat and light into the human body might be an effective disinfectant. Doing so, says Setlow, “would kill the Covid but you would kill the person.” Trump later walked back that recommendation.
Convinced that technology can be an important tool against Covid-19, a number of companies are pushing ahead. One that reports its product can kill SARS-CoV-2 is Xenex Disinfection Services, Inc., which makes R2-D2-like germ-zapping robots that are primarily used in health care facilities. These robots use a xenon lamp to emit pulses of broad-spectrum, high-intensity UV light that disinfect a room. According to Xenex CEO Morris Miller, tests by the Texas Biomedical Research Institute, an independent research entity, showed the robot could deactivate SARS-CoV-2 in two minutes. He says the robots are currently in over 500 hospital facilities, including one in Bergamo, the epicenter of Italy’s epidemic. The robots are also being used in hotels and government buildings, he adds, and airlines have expressed interest. Each Xenex robot costs $125,000, with a life expectancy of five to seven years.
PuraCath Medical, Inc. is focused on reducing hospital-acquired infections with a handheld UV ray device that disinfects catheters. The device, called the Firefly, zaps the part of the catheter that connects to medication or other solutions. In February, PuraCath received a $3 million collaborative grant from the National Institutes of Health to test the Firefly on SARS-CoV-2 and other microbes. In a test that used a sample of Covid-19 from a patient in Washington state, the Firefly successfully killed the coronavirus within one second. The device hasn’t, however, been cleared by the U.S. Food and Drug Administration, so it isn’t yet commercially available. In the meantime, PuraCath is also working on a device to disinfect N95 or equivalent medical-grade masks, 12 at a time. “Given the encouraging data [on] disinfecting through lots of layers through a catheter, we are confident we can disinfect a mask,” says Julia Rasooly, the company’s CEO and president. That device is expected to be ready later this year.
On May 19th, the New York Metropolitan Transit Authority launched a $1 million pilot project to test the use of UV-C rays in disinfecting subways, buses, and other forms of transit. Mark Dowd, the MTA’s chief innovation officer, says he hopes disinfection will “provide reassurance for people to start using the subways and buses.” The project involves 150 mobile disinfecting units developed by Puro Lighting to disinfect vacant spaces. Brian Stern, Puro’s CEO, says that his company uses the same type of light as Xenex but overcomes the steep cost by using a miniaturized version. He says the lamp’s small size results in a lower-cost product that ranges from a few thousand dollars to $20,000, depending on the size of the system.
Nardell believes UV-C can be effective for disinfecting spaces in large institutions, though he cautions that the true test will be how it works outside the laboratory. The Illuminating Engineering Society report made clear that UV-C can’t disinfect some surfaces. “Anything that’s shadowed behind dirt or dust, doesn’t get hit by the photons and inactivated,” Nardell said. “It’s important to have the right intensity of light and lots of overlapping fields of light so you eliminate the possibility of shadows, and light comes from multiple directions.”
Stern argues that cost and availability have been major obstacles to widespread adoption of the technology. “The majority of the commercial-grade technology in the market prior to the pandemic was in the form of the UV pushcarts or ‘robots,’ which range in retail price from $55,000 to $145,000,” he says, noting that the health care industry was one of the few that could afford these prices.
Patti Costello, executive director of the Association of the Health Care Environment, an arm of the American Hospital Association, says research on UV-C for disinfection has shown some promising results, but more studies need to be conducted. Since the technology isn’t yet formally recognized as an antimicrobial agent, she adds, “widespread use will take time.” She agrees with Stern that high costs to purchase and maintain the devices are another barrier.
Safety remains another key obstacle. Exposure from the current UV-C ray technology, notes Setlow, can damage the skin and eyes when used indoors.
David Brenner, director of the Center for Radiological Research at Columbia University, is investigating a specific UV-C wavelength, 222 nanometers, that could address the issue of human safety. This wavelength is known as Far-UVC. Brenner says his research indicates that Far-UVC cannot reach the epidermis or the cornea. “It can’t reach any living cells in our body,” Brenner said in an email. Setlow says that Far-UVC technology “offers the potential to disinfect while people are there,” but he emphasizes that definitive safety data is required before this technology can take off.
Nardell, who was previously infected with Covid-19, is nevertheless optimistic that Far-UVC will make inroads to prevent others from suffering the same fate. His ideal application for this technology in the near future would be to aim it directly over a coffee bar or in a nail salon between the technician and the customer. “It’s going to be revolutionary,” he says. “You’re going to see it everywhere.”